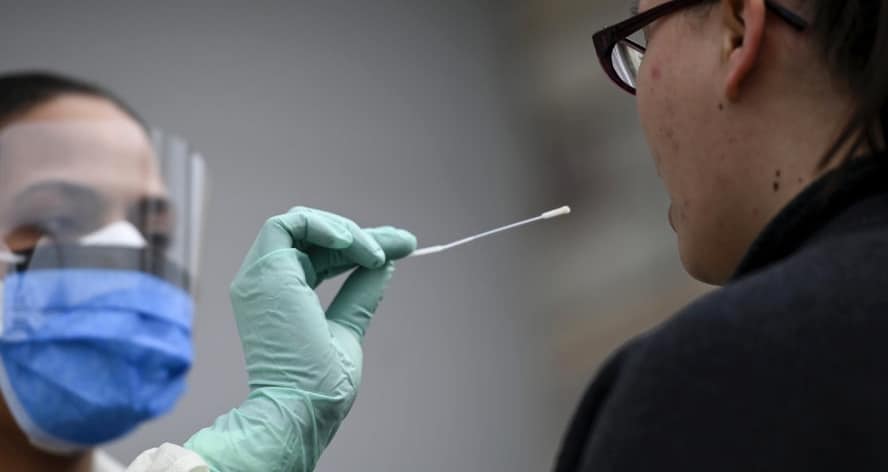
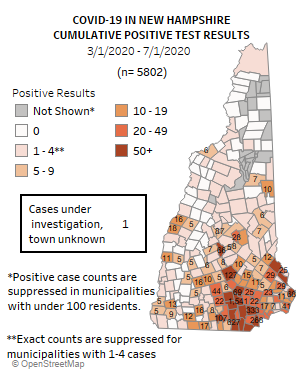
COVID-19 testing remains critical to help treat, isolate, or hospitalize people who are infected. Nearly 120,000 people have been tested in New Hampshire.
“When a communicable disease outbreak begins, the ideal response is for public health officials to begin testing for it early”, informs Dr. Eduardo Sanchez, American Heart Association’s chief medical officer for prevention.
That leads to quick identification of cases, quick treatment for those people, and immediate isolation to prevent spread. Dr. Sanchez says that early testing also helps to identify anyone who came into contact with infected people so they too can be quickly treated.
COVID-19 is disproportionately affecting Hispanic, Latino, and Black communities across the country. In New Hampshire, those two groups make up about 17-percent of total coronavirus cases statewide, but account for just a little over 5-percent of the state’s population.
“We know in particular with our populations of color, those disparities have existed for decades,” Bobbie Bagley, Nashua’s public health directors told NHPR. “And so we need to make sure that we have a particular focus on addressing those needs so that we can close those gaps and improve the health outcomes for that population group.”
Bagley said that her team pays close attention to “social determinants of health” — factors beyond someone’s medical history that play a big role in shaping their health outcomes. This includes things like where someone lives, how much they earn, and if they’re a racial or ethnic minority in this country.
Similarly, the Connecticut Health Foundation advised that as this disease unfolds, it is important to recognize the roots of these disparities including differences in access to health care, unequal treatment within the health care system, unequal access to resources such as stable housing and healthy food, and personal experiences of discrimination and racism that have lasting physical and mental health consequences.
Some key facts:
- Having a regular source of care is a key factor in staying healthy; now, it also means having a place to call if you feel sick and wonder if you need to be tested for COVID-19. Yet in 2018, 33% of Hispanic residents and 23% of black residents did not have a personal doctor (by contrast, only 11% of white residents reported not having a personal doctor).
- Research has also found that black and Hispanic patients are at risk of receiving less aggressive treatment than white patients. For example, studies found that Hispanic patients were half as likely to be given pain medication when they went to the emergency room with a broken bone, and black children and teens with appendicitis were significantly less likely to be given opioids to treat pain. Among patients with heart issues, black patients were significantly less likely than white patients to receive interventions that could promote long-term survival.
- Research has also linked experiencing racism and discrimination with a wide range of negative physical and mental health consequences including depression, anxiety, hypertension, breast cancer, and giving birth preterm or having a low-birthweight baby. One way discrimination could lead to poorer health is through repeated activation of the body’s stress response system, which can have negative long-term physical and psychological effects.
The rate of positive COVID-19 tests in the Granite State has remained at about 2% to 3% over the past few weeks, noted by Dr. Benjamin Chan, the state epidemiologists.
Amid improving overall COVID-19 infection trends in the Granite State, health officials urged people this week to continue wearing masks and maintaining social distancing.
Governor Chris Sununu echoed the call for Granite Staters to wear masks when out in public. He called it a commonsense way to protect the community and help ensure that New Hampshire doesn’t have to reverse its reopening plans, reported WMUR.
“Wear your mask where you cannot socially distance,” Sununu said. “It works. It’s been proven to work time and time again.”